Diabetic Retinopathy
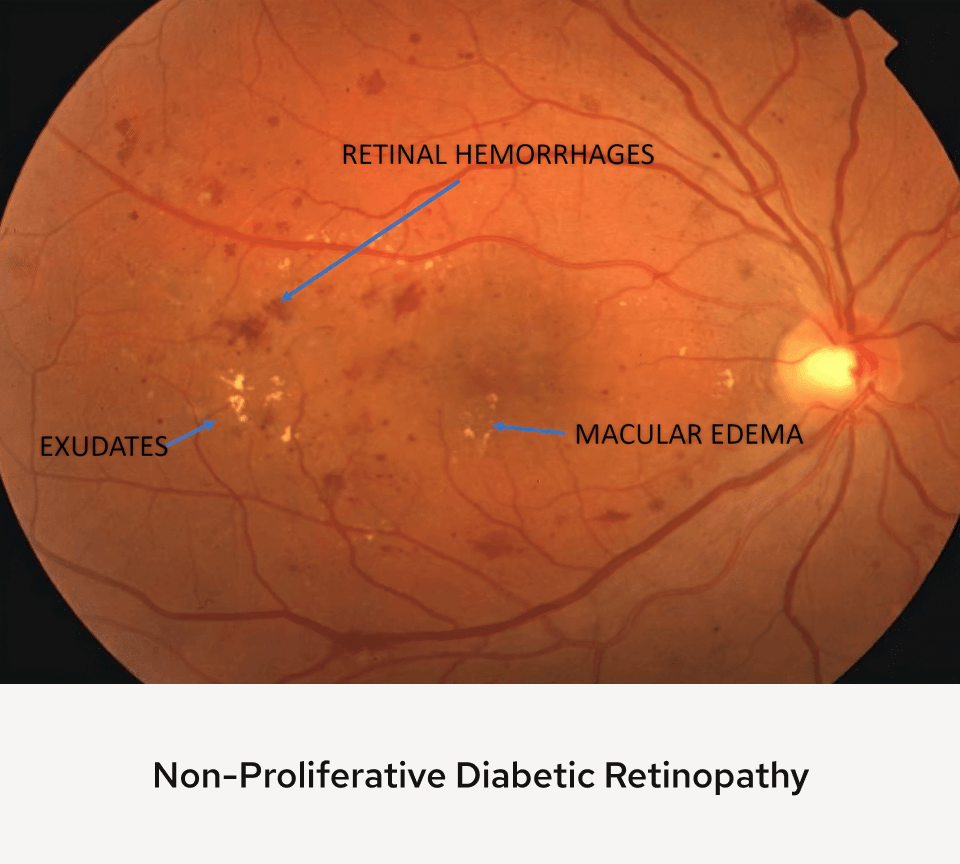
Diabetes mellitus is a disorder caused by a deficiency in insulin (Type 1) or an inability of existing insulin (Type 2) to keep blood sugars under control. Over time, patients with diabetes, especially those with poorly controlled blood sugar may develop eye, kidney, heart, nerve and skin problems. In the eye, diabetes mainly affects the retina and causes diabetic retinopathy. Diabetes affects small blood vessels all over the body and makes them weak and leaky. In the retina, capillaries (the tiniest of blood vessels) that supply nutrients and remove waste products become leaky and allow contents of blood (serum, lipids, and blood cells) to leak into the retina, causing the retina to swell (edema).
This stage of retinopathy is called non-proliferative diabetic retinopathy. When swelling occurs in the macula (the part of the retina responsible for color and fine vision), vision becomes blurred and permanent damage can occur to the retina. We examine your eye to determine if there is swelling in the macula that requires treatment (clinically significant macular edema). For mild cases, treatment can be performed with laser in the office. When it becomes more severe, we have the option of injecting anti-VEGF (vascular endothelial growth factor) medications or steroids. In a few cases, vitrectomy surgery (removal of the vitreous gel) may be necessary, especially if laser and medications have failed.
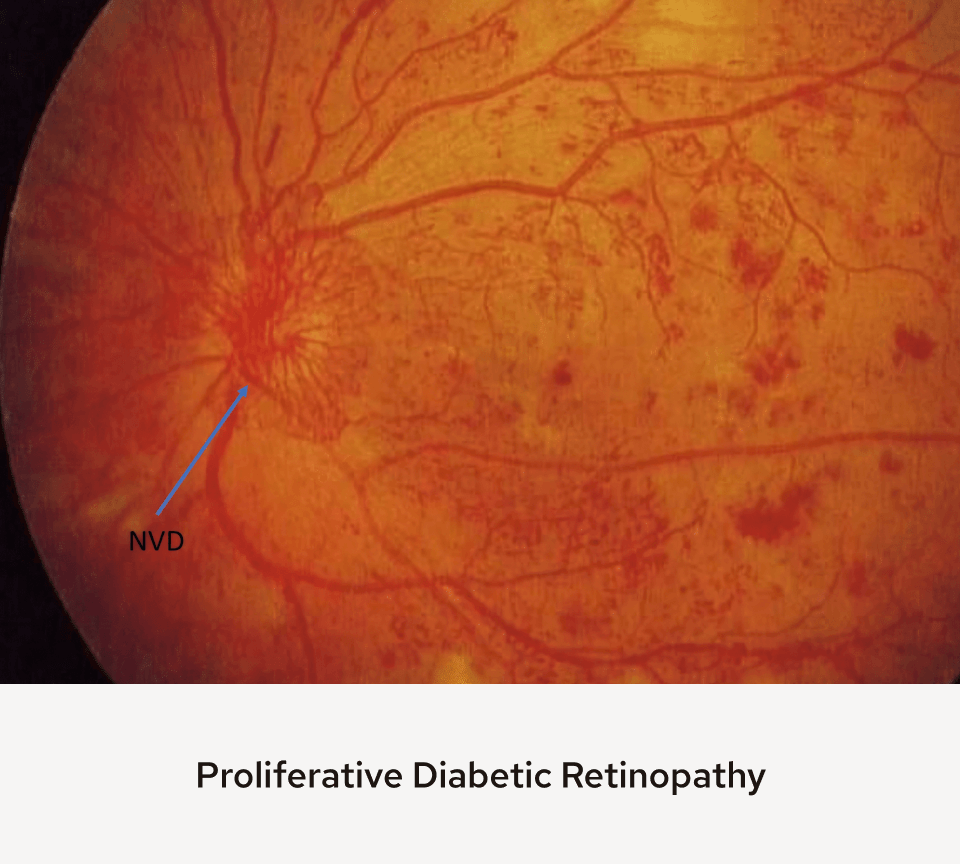
In more severe cases of diabetic retinopathy, leaky capillaries may become permanently damaged and may not work at all. This capillary damage results in lack of blood flow to sections of the retina (ischemia). Ischemia results in the production of chemical messengers in the retina that lead to development of abnormal new blood vessels (retinal neovascularization) that can grow out of the retina and into the vitreous (the jelly like substance that fills the eye). This is called proliferative diabetic retinopathy (PDR).
Unfortunately, these new blood vessels are not helpful. They are fragile and can bleed causing the back of the eye to fill with blood causing string-like floaters, then hazy, and loss of vision. These abnormal blood vessels also grow with a scar tissue that can begin to pull on the retina and lead to a retinal detachment. At this stage, surgery is often required and if not caught in time, this can lead to permanent loss of vision.
Much of the changes and damage that occur with diabetic retinopathy happen before any symptoms develop so it’s important to have routine eye exams if you have diabetes. Plus, the disease is much easier to treat if caught early. PDR can be treated with laser in the office or with the injection of anti-VEGF (vascular endothelial growth factor) medications.
The most important way to prevent vision loss in diabetes is to keep blood sugars and blood pressures under good control. Keeping the hemoglobin A1C (long term measure of sugar control) under 7.0 is extremely important. Tight blood sugar control reduces the risk of developing diabetic retinopathy.
Even if retinopathy develops, patients with tight control tend to have mild and non-sight threatening retinopathy. Annual check-ups by your eye doctor or retina specialist after the diagnosis of diabetes and more frequent follow-up evaluation once diabetic retinopathy develops is important. Women who have diabetes and become pregnant may need very close monitoring during pregnancy.
Schedule a Consultation for Diabetic Retinopathy
The retina specialists of AVRUC provide expert care for diabetic retinopathy. With convenient retina center locations in Carmel, Bloomington, Muncie, and Avon, we welcome patients from the greater Indianapolis area, Evansville, Lafayette, Terre Haute, and beyond.

